Important note before reading: O2 Dental Group does not offer subperiosteal implants. This article is provided for informational purposes only — to help patients with complex bone loss understand what this option is, when it enters the conversation, and what questions to bring to any provider evaluating their case. If you’d like to discuss your implant options at O2 Dental Group, we offer comprehensive 3D-guided implant consultations to evaluate what paths are realistic for your specific anatomy.
Most patients don’t start the implant conversation here. They start with a simpler hope: that standard implants will work, that enough bone remains, that the path back to a stable smile will be more straightforward than they feared.
When imaging shows otherwise, the emotional weight of that shift is real. Bone loss changes the conversation quickly. A patient who came in to discuss replacing missing teeth is suddenly navigating anatomy, grafting timelines, surgical burden, and a set of options that felt abstract until they became personal.
Subperiosteal implants are one of the options that sometimes enters this conversation — and one of the least well understood. What follows is a clinically grounded explanation of what they are, what the current evidence says about them, and why the most important question is never simply whether something can be done.
What Subperiosteal Implants Are — and How They Differ from Standard Implants
To understand subperiosteal implants, it helps to start with what most people already know about standard implants.
Conventional endosteal implants are titanium posts placed directly into the jawbone. They rely on osseointegration — the process by which bone fuses to the implant surface over time — to create a stable foundation for the final restoration. This process requires adequate bone volume and density at the implant site. When sufficient bone is present, endosteal implants are the standard of care and have decades of well-documented outcomes supporting their use.
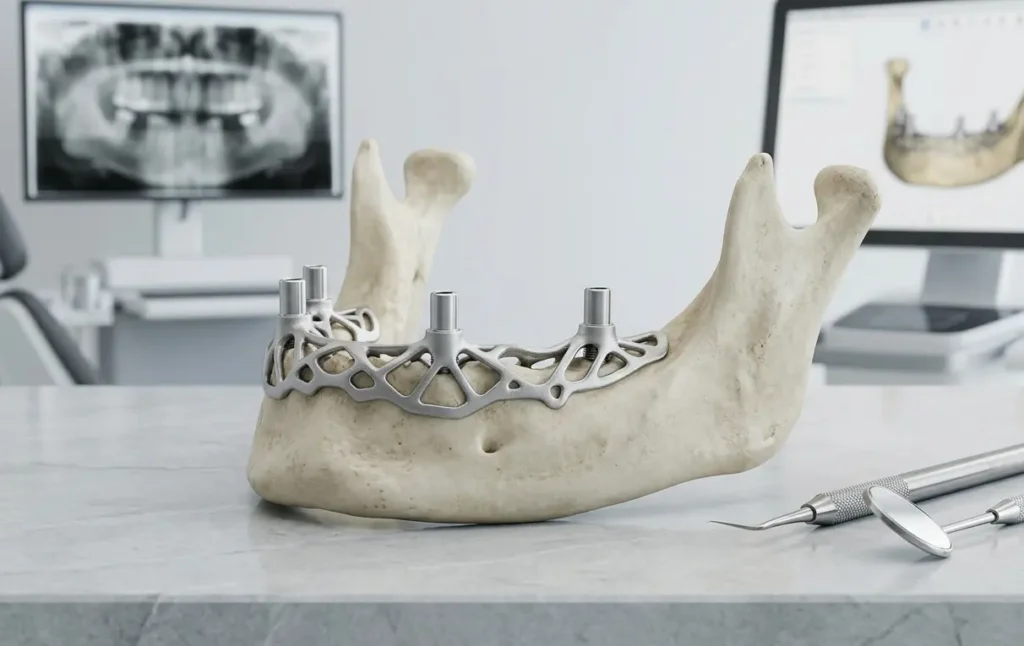
Subperiosteal implants work on a fundamentally different principle. Rather than being placed into the bone, they use a custom-fabricated metal framework that rests on top of the jawbone, positioned beneath the periosteum — the connective tissue layer that covers the bone surface. Posts from this framework extend through the gum tissue to support the prosthetic restoration above.
The problem they’re designed to address is specific: patients whose available bone is so reduced in volume, so thin, or so anatomically limiting that placing standard implants into the bone is not straightforward — or not possible without extensive surgical reconstruction first. In these cases the issue isn’t simply missing teeth. It’s that the structural foundation those teeth would normally rely on has been significantly compromised.
Why Subperiosteal Implants Are Being Discussed Again
Subperiosteal implants are not a new concept. The category has existed since the mid-twentieth century, and for a significant period they largely fell out of favor as endosteal implant systems improved and bone grafting techniques became more predictable. The older generation of subperiosteal implants carried well-documented concerns — soft tissue complications, mechanical failures, and outcomes that compared unfavorably with endosteal alternatives when grafting made those alternatives possible.
The renewed clinical interest in subperiosteal implants is driven by what has changed in how they’re designed and planned. The American Association of Oral and Maxillofacial Surgeons describes modern subperiosteal implants as a digitally driven treatment possibility for severe alveolar atrophy and anatomical limitations. Recent literature makes the same point: digital imaging, computer-aided design and manufacturing, and patient-specific fabrication have meaningfully changed the precision and customization available in these cases.
A custom framework designed from cone beam CT imaging and digital planning is a different clinical proposition from the older generation of devices. That doesn’t mean the old concerns disappeared. It means the category evolved — and deserves evaluation on current evidence rather than on the reputation of an earlier iteration.
When Subperiosteal Implants Enter the Treatment Discussion
Most patients with bone loss do not need subperiosteal implants, and it’s important to say that clearly at the outset.
Bone loss exists on a spectrum. Many patients with reduced bone volume remain candidates for conventional endosteal implants, with or without bone grafting, depending on what 3D imaging reveals about the actual available anatomy. Full-arch implant solutions, sinus augmentation, and other approaches may be appropriate depending on the specific presentation. Bone loss does not automatically redirect a patient toward subperiosteal implants.
Subperiosteal implants typically become relevant in a narrower set of circumstances:
Severe alveolar atrophy — bone that has resorbed to the point where conventional implant placement is not achievable without major reconstruction, if at all.
Prior grafting failure — patients who have already undergone bone grafting that did not achieve the volume needed for endosteal implant placement.
Anatomical limitations — specific jaw anatomy that restricts where standard implants can be safely placed regardless of available bone volume.
High surgical burden — patients, particularly older or medically complex patients, for whom the staged surgical process of major grafting followed by implant placement represents a burden that outweighs the benefits of that pathway.
Patient preference against extensive reconstruction — some patients, fully informed of their options, prefer to avoid a lengthy staged reconstruction when an alternative path to restoration exists.
None of these factors alone determines whether subperiosteal implants are the right answer. They determine whether the option belongs on the table for evaluation. The difference matters.
What the Current Evidence Actually Says
The clinical literature on modern subperiosteal implants is encouraging but explicitly preliminary — and it’s worth understanding that distinction before drawing conclusions from it.
A 2024 review described customized subperiosteal implants as promising for edentulous patients with atrophic jaws, reporting strong short-term survival rates in the available literature. The same review was careful to note that the scientific evidence base remains limited and that rigorous long-term follow-up data is still needed. A 2025 review echoed this assessment — describing modern subperiosteal implants as a promising option for extreme jaw atrophy while emphasizing the critical importance of patient selection and soft tissue management.
What this means practically: the early and mid-term outcomes in carefully selected patients look favorable. What it doesn’t mean: that long-term durability is established at the level it is for conventional endosteal implants, which have decades of well-documented outcomes across large patient populations.
For patients evaluating this option, the honest framing is this: the evidence is sufficient to justify consideration in appropriate cases. It is not sufficient to justify enthusiasm that outpaces the data. Careful patient selection isn’t a bureaucratic hurdle before treatment — it is itself part of what makes the treatment work.
The Real Benefits — and the Real Tradeoffs
For a patient whose anatomy genuinely limits conventional implant options, subperiosteal implants may offer something clinically meaningful: a path to implant-supported restoration that doesn’t require — or doesn’t solely require — the extensive bone reconstruction that would otherwise be necessary. For selected patients this can mean a shorter overall treatment timeline and a plan that feels achievable rather than exhausting.
The tradeoffs are real and deserve direct acknowledgment.
Soft tissue complications are consistently noted in the literature as a concern specific to the subperiosteal design. The framework sits on the bone surface rather than within it, and the tissue response over time requires careful management.
Prosthetic complications have been documented in available studies, including a 2024 CAD-CAM subperiosteal implant study that reported favorable rehabilitation outcomes alongside complications requiring clinical management.
Maintenance demands are ongoing. This is not a restoration that functions without continued attention to tissue health, bite forces, and follow-up care. AAOMS includes both soft tissue and mechanical complications in its practical framework for evaluating these cases.
Evidence maturity remains a legitimate consideration. Conventional endosteal implants have a significantly larger and longer evidence base. Subperiosteal implants in their modern form are still accumulating the kind of long-term data that would allow more definitive outcome statements.
None of these tradeoffs are reasons to categorically dismiss the option. They are reasons to enter the evaluation with accurate expectations rather than with hope that complexity has been solved.
The Questions Worth Asking at Any Implant Evaluation
Because O2 Dental Group does not provide subperiosteal implants, the purpose of this section is specifically to help patients who are exploring this option elsewhere ask the right questions — and to help patients consulting with O2 understand what a thorough implant evaluation looks like regardless of which path ultimately makes sense.
A complete evaluation for any complex implant case should address:
Bone volume and anatomy — how much bone is actually present, where, and what that means for each option on the table. This requires 3D cone beam CT imaging, not standard two-dimensional X-rays.
Conventional Endosteal Implants: These are titanium posts placed directly into the jawbone. They rely on osseointegration — the process by which bone fuses to the implant surface. This requires adequate bone volume. When sufficient bone is present, dental implants are the standard of care.
Alternative full-arch options — whether solutions using fewer strategically placed implants to support a full-arch restoration are appropriate given the available anatomy.
Surgical suitability — whether the patient’s overall health, medications, and medical history support the surgical approach being considered.
Restorative goals — what the final restoration needs to accomplish functionally and aesthetically, and how each option performs against those goals.
Long-term maintenance — what ongoing care the restoration requires and whether that’s realistic for the patient’s situation.
Provider experience — for subperiosteal implants specifically, the digital planning, fabrication, and surgical placement require experience with the specific technique. This is not a case type where general implant experience is sufficient preparation.
The problem they’re designed to address is specific: patients whose available bone is so reduced in volume or so thin that placing standard implants is not possible without extensive bone grafting or surgical reconstruction.
What O2 Dental Group Offers for Complex Implant Cases
Again — subperiosteal implants are not a service O2 Dental Group provides. Patients who have been advised that subperiosteal implants may be appropriate for their case should seek evaluation with an oral and maxillofacial surgeon or prosthodontist with specific experience in this treatment.
What O2 Dental Group does offer for patients with bone loss or complex implant situations is a thorough evaluation using cone beam CT imaging and digital planning to determine what options are actually available given the specific anatomy — including conventional endosteal implants with or without grafting, full-arch implant solutions, and other appropriate pathways depending on what the imaging shows.
The goal of that evaluation is never to fit a patient into a predetermined answer. It is to understand what the jaw can support, what the patient’s health and goals require, and which path offers the most realistic combination of stability, function, and long-term confidence.
If you’ve been told your case is complicated — by bone loss, prior failed treatment, or anatomy that has limited your options elsewhere — that conversation is exactly what O2’s implant consultations are designed for.
Frequently Asked Questions
What are subperiosteal implants?
A subperiosteal implant is a custom-fabricated metal framework placed on top of the jawbone, beneath the periosteum, with posts extending through the gum tissue to support a prosthetic restoration. Unlike conventional implants, they don’t require placement into the bone — which is why they’re considered in cases of severe bone loss.
Does O2 Dental Group offer subperiosteal implants?
No. O2 Dental Group does not provide subperiosteal implants. This article is informational. Patients who have been advised that subperiosteal implants may be appropriate should consult with an oral and maxillofacial surgeon or prosthodontist with specific experience in this treatment.
Who are subperiosteal implants designed for?
Patients with severe jawbone atrophy or anatomical limitations that make conventional implant placement difficult or impossible without extensive reconstruction. They are a specialized option for selected complex cases — not the standard implant recommendation for most patients with bone loss.
Are subperiosteal implants common?
No. They represent a small subset of implant cases and are typically considered only after conventional implant pathways have been evaluated and found to be significantly limited by the patient’s anatomy.
How are modern subperiosteal implants different from older designs?
Modern subperiosteal implants are designed using cone beam CT imaging, digital planning software, and CAD/CAM fabrication — producing patient-specific frameworks with significantly greater precision than earlier generations. This technological evolution is the primary driver of renewed clinical interest.
What does the evidence say about their outcomes?
Early and mid-term outcomes in carefully selected patients are described as promising in recent reviews, including a 2024 review and a 2025 review both noting favorable results in atrophic jaw cases. Both reviews also emphasized that the evidence base is still limited and that long-term data continues to be needed. Conventional endosteal implants have a substantially more mature evidence base.
What are the risks?
Soft tissue complications, prosthetic mechanical issues, and ongoing maintenance demands are consistently noted in the literature. A 2024 CAD/CAM subperiosteal implant study reported favorable outcomes alongside documented complications requiring management. These are not reasons to avoid the option in appropriate cases — they are reasons to enter it with accurate expectations.
What should I do if I’ve been told I’m not a candidate for regular implants?
Start with a thorough 3D evaluation. Many patients who have been told conventional implants aren’t possible have not had cone beam CT imaging interpreted by a provider experienced in complex implant planning. The anatomy revealed by 3D imaging frequently opens options — including conventional endosteal implants with appropriate grafting or full-arch solutions — that weren’t visible on standard X-rays.
O2 Dental Group offers comprehensive implant consultations using cone beam CT imaging and digital planning for patients with straightforward and complex implant needs. If you’ve been told your case is complicated, contact us to schedule an evaluation and discuss what options are realistic for your specific anatomy.