Oral Surgery Wilmington, NC
Oral surgery (maxillofacial surgery) refers to procedures performed by a dental specialist on oral structures such as the mouth, jaw, gums, and teeth.
Various conditions that affect the oral cavity, face, and neck can only be corrected through oral surgery. They include:
- Missing and broken teeth
- Impacted teeth
- Jaw misalignment
- Facial trauma
- Sleep apnea
- Oral cancer
- Oral cysts and tumors
Common Types of Oral Surgery
Wisdom Teeth Extraction
Wisdom teeth emerge in the late teenage years or early twenties. These sets of teeth develop last and can cause dental complications if you don’t have enough room left in the jaw to accommodate the extra teeth.
The lack of jaw space may lead to impaction, where the wisdom teeth fail to emerge properly and remain trapped beneath the gum line. An impacted wisdom tooth can cause severe pain, inflammation, and damage to the surrounding teeth.
Your dentist may recommend tooth extraction to extract the impacted wisdom teeth and address the health complications.
Facial Trauma Repair
Facial trauma refers to injuries to facial and oral structures. This can be a result of violence, sports-related injuries, and accidents. Facial trauma can cause facial bone fractures, muscle lacerations, soft-tissue damage, and nerve impairment.
In most cases, oral surgery may be the only way to repair facial trauma damage and restore functionality to the affected oral and facial structures. Your dentist may recommend the following facial trauma repair procedures depending on your situation:
- Orbital fracture repair: This surgical procedure involves realigning fractured orbital bones to preserve eye function. The surgeon may use plates, screws, and wires to realign and stabilize the affected orbital bones.
- Soft tissue repair: This procedure addresses facial soft tissue damage such as burns and lacerations. The surgeon may use techniques such as suturing and specialized adhesive products to close the wound and promote healing.
- Dental trauma repair: Dental injuries such as broken or missing teeth are a typical result of facial trauma. Dental trauma repair involves correcting teeth misalignment and replacing missing teeth with dental prosthetics.
- Facial bone fracture repair: Facial trauma can result in broken or fractured jaw bones and cheekbones. Your surgeon may use biocompatible surgical plates to stabilize and realign the affected facial bones.
Dental Implants
Dental implants are a type of oral surgery procedure that addresses tooth loss. The treatment involves embedding threaded posts into the jaw as artificial tooth roots. The threaded posts are made from medical-grade titanium and act as support structures for replacement teeth or dental prostheses such as crowns and bridges.
Dental implants are a popular teeth replacement solution since they are long-lasting and provide a functional and natural-looking alternative for missing teeth.
Jaw Surgery
Jaw surgery is a corrective surgical procedure that addresses functional and aesthetic irregularities affecting the jaw bones, facial skeletal structure, and teeth. Jawbone irregularities can cause facial imbalance, jaw pain, and malocclusion (misalignment of the teeth).
Corrective jaw surgery may involve:
- Modifying the size of the jawbones
- Reshaping the chin
- Correcting misaligned teeth
- Repositioning the upper or lower jaw
Your dentist may recommend jaw surgery to correct jaw misalignment, improve facial symmetry, improve chewing function, and help enhance your speech.
Gum Grafting
Severe periodontitis can cause a recession of the gums around the affected tooth. Gum recession leaves the tooth exposed, increasing the chances of tooth loss, progressive tooth decay, and tooth sensitivity.
Gum grafting is an oral surgical procedure that involves taking gum tissue from a healthy area of the mouth, such as the roof of the mouth, and grafting it onto the affected gum tissue.
The gum graft regenerates the damaged gums, preventing further gum recession and improving the overall health of the gum line.
Temporomandibular Joint (TMJ) Surgery
The temporomandibular joint (TMJ) connects the lower jaw to your skull. The TMJ is responsible for jaw movement when speaking, chewing, and talking. TMJ disorders can cause jaw stiffness, chronic pain, limited jaw mobility, severe neck pain, and toothaches.
Oral surgery may be the only way to address severe cases of TMJ disorders, especially if other treatments are unsuccessful. Your dentist may recommend one of the following TMJ surgical procedures depending on your symptoms and diagnosis:
- Arthroscopy: This surgical procedure involves inserting a small camera through an incision in front of the ear. The video feedback allows the surgeon to visualize your TMJ and determine the best way to resolve TMJ pain. Treatment options include removing inflamed tissue, smoothing rough joint surfaces, realigning the disc, or removing adhesions in the joint.
- Arthrocentesis: This non-invasive procedure addresses locked jaw and reduced jaw mobility. The surgeon inserts a needle filled with a saline solution into the TMJ and flushes the joint space. Arthrocentesis can help restore jaw function by washing out debris from the TMJ and reducing inflammation.
- Open-joint surgery: This oral surgical procedure addresses severe cases of TMJ disorders. It involves accessing the TMJ directly and using surgical techniques such as implant placement, tissue removal, and joint replacement to repair the TMJ.
Oral Surgery Procedures
Preparation for Oral Surgery
Ask Questions.
Don’t hesitate to ask questions. Request an appointment with your surgeon and let them know of any concerns or questions you may have regarding your procedure.
Follow Pre-op Instructions
Carefully read the pre-op instructions provided by your surgeon. The instructions may contain specific information to help you prepare for the surgery and avoid complications.
Arrange Transportation
It would be best to arrange transportation to and from your surgical appointment. Most oral surgical procedures require anesthesia which makes driving post-op unsafe.
Dress Appropriately
Go for loose and comfortable clothes on the day of the procedure. Also, avoid long sleeve shirts, as technicians will have difficulty setting up your IV and monitoring your vitals.
Avoid Food and Drink
Don’t eat or drink for at least eight hours before the procedure. Fasting reduces the risk of aspiration (your stomach content filling the lungs) during surgery.
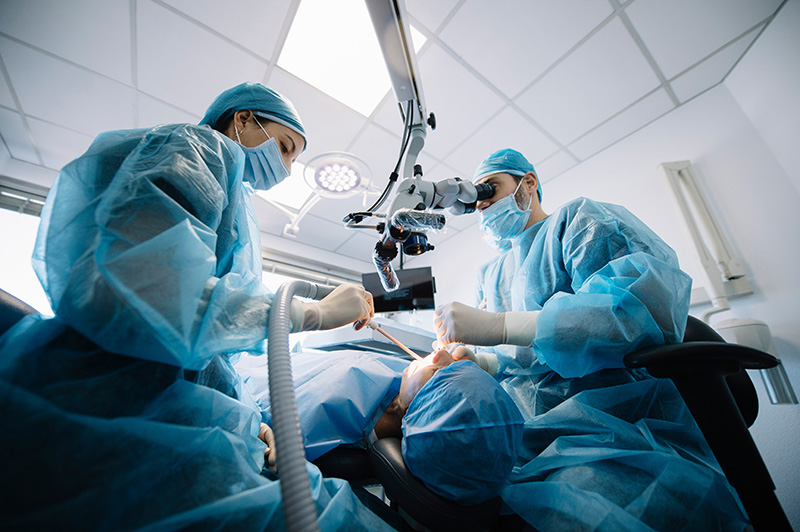
What to Expect During the Procedure
Anesthesia Administration
Your oral surgeon administers anesthesia depending on your diagnosis, type of surgery, and preference. Common types of anesthesia used in oral surgeries include:
- Local anesthesia: This type of anesthesia is used in standard oral procedures like tooth extractions and root canals. It’s injected into the surgical site, temporarily blocking nerve pain signals and allowing you to stay awake during the surgery
- General anesthesia: A type of anesthesia that puts you in a state of unconsciousness. It’s used in complex oral surgical procedures such as orbital fracture repair
- Sedation anesthesia: A type of anesthesia that induces a relaxed state during the surgical procedure. The surgeon may recommend sedation anesthesia to help you overcome dental anxiety during minor surgical procedures
- Regional anesthesia: A potent anesthesia that numbs large face areas during complex procedures. For instance, your surgeon may recommend regional anesthesia for some TMJ surgeries
Incision
Next, your surgeon makes an incision in the surgical site depending on the procedure. This step may not be necessary for minor operations such as tooth extractions.
Repair
The surgeon makes corrections to the affected area. This may involve realigning fractured bones, removing damaged tissue, or stabilizing weak facial structures.
Closure
Your surgeon closes the incision using stitches or sutures after completing the procedure to ensure proper healing and prevent the risk of infection.
Recovery and Aftercare for Oral Surgery
The recovery period after oral surgery depends on the type of surgery, your regenerative capacity, and your postoperative care routine. For instance, minor surgical procedures like tooth extractions and root canals may heal in a few days.
Complex surgical procedures such as facial trauma repair and open-joint surgery may take several weeks to heal fully. It’s important to note that your postoperative care routine plays a significant role in the healing process.
Your oral surgeon may recommend the postoperative care tips below to care for the surgical site, promote healing and avoid complications.
- Avoid smoking: Smoking wreaks havoc on oral structures and reduces regenerative capacity. Cigarette smoke also increases the risk of infection.
- Apply ice packs: Applying ice packs on the surgical site for a few minutes each day can help reduce swelling, pain, and discomfort.
- Take medication as directed: Your surgeon may prescribe pain medication and antibiotics. Following the prescriptions will help with pain management and reduce the risk of infection.
- Watch your diet: Observe a diet of soft, cool foods such as yogurt, smoothies, applesauce, and pudding. Avoid spicy, crunchy, and hot foods, which may irritate the surgical site.
- Follow-up appointments: Be sure to attend follow-up appointments with your surgeon. They’ll examine your progress and address any complications with the surgical site.
- Maintain good oral hygiene: Maintaining good oral hygiene after your surgery promotes healing and reduces the risk of complications. However, brush and floss gently to avoid irritating the surgical site.
- Rinse with saline water: Gently rinsing your mouth with warm saline water can reduce discomfort and the risk of infection.
Oral Surgery Complications
Potential complications of oral surgery include:
- Nerve damage: Though rare, oral surgery can result in temporary or permanent nerve damage. You should consult your surgeon immediately if you notice tingling or loss of sensation in the face.
- Infection: Bacteria may infiltrate your body through the incision site, causing infection. Contact your surgeon if you develop a fever, discharge from the incision site, and swelling.
- Excessive bleeding: While bleeding is normal after oral surgery, excessive bleeding that persists after several hours is not a good sign.
- Dry socket: This is a condition where the protective blood clot that forms after a tooth extraction is dislodged. As a result, the tooth socket becomes exposed, increasing the risk of infection and causing severe pain.
It’s important to note that adhering to the postoperative care instructions given by your surgeon drastically reduces the risk of developing complications.
Alternatives to Oral Surgery
Your dentist may recommend the following alternatives to oral surgery depending on your diagnosis and individual preference:
- Orthodontic appliances: Your dentist may recommend braces and clear aligners to correct teeth misalignment and bite issues.
- Antibiotics: Mild cases of gum infection can be treated using antibiotics and other medication.
- Root canal therapy: This procedure prevents the need for tooth extraction. Your dentist will remove infected pulp tissue, replace it with a biocompatible material and save the natural tooth.
- Laser therapy: This cutting-edge, non-surgical procedure uses lasers to treat gum conditions like gingivitis preventing the need for invasive surgical procedures.
Oral surgery may sound intimidating, but understanding the various procedures helps you know what to expect and promote healing through proper surgical site care. Consult a skilled dental professional to learn more about oral surgery and alternative treatment options.
Schedule Today!
We look forward to meeting you. Call (910) 377-6453 or request an appointment online to set up your first visit. We’ll be in touch soon.
O2 Dental Group of Wilmington
(910) 377-6453
Monday:
Tuesday:
Wednesday:
Thursday:
Friday:
Saturday:
Sunday:
8:00am – 4:00pm
8:00am – 4:00pm
9:00am – 6:00pm
9:00am – 6:00pm
8:00am – 2:00pm
CLOSED
CLOSED

