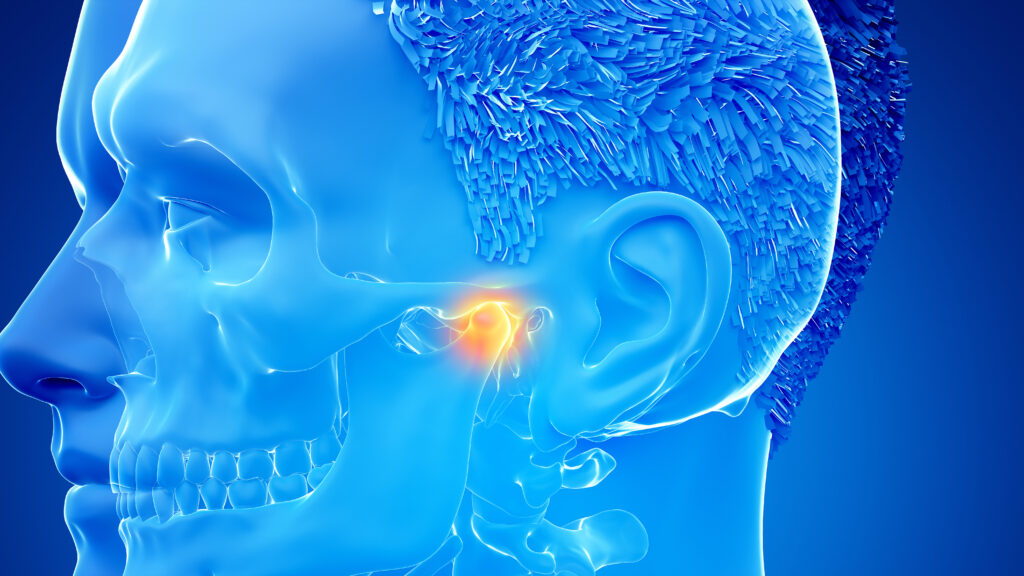
The Temporomandibular Joint, often abbreviated as TMJ, serves as a pivotal connection between your jaw and the temporal bones of your skull. This intricate joint plays a crucial role in our daily lives, facilitating essential functions such as speaking, chewing, and yawning. However, when complications occur within this joint, they give rise to a condition known as Temporomandibular Joint Disorder, commonly referred to as TMJ disorder or simply TMJ.
What is TMJ?
TMJ disorders represent a collection of conditions that impact the hinge-like joint connecting your jaw to your skull. This joint, functioning much like a sliding hinge, orchestrates a range of movements within your mouth. These movements include everything from the simple opening and closing of your mouth to more complex lateral or side-to-side motions.
When this joint deviates from its normal functioning, it can lead to discomfort and restricted movement in the jaw area and surrounding muscles. Such disorders can manifest as temporary conditions that resolve without extensive treatment, or they can persist over the long term, necessitating professional intervention. The intensity of symptoms can fluctuate significantly among individuals, spanning from mild discomfort to severe pain. It’s also noteworthy that TMJ disorders can affect either one or both sides of your face.
While ‘TMJ’ is a widely recognized and used term, the more precise terminology for disorders affecting the Temporomandibular joint is TMD or Temporomandibular Disorders. However, to facilitate common understanding, ‘TMJ’ continues to be the prevalent term used to describe these conditions.
Causes and Symptoms of TMJ Disorders
The root of TMJ disorders can be elusive, often stemming from a combination of factors such as genetic predisposition, physical trauma, or underlying conditions like arthritis. Certain behaviors, like teeth grinding or clenching, often stress-induced, can place undue pressure on the joint, accelerating its deterioration.
In some cases, the displacement of the soft cushion or disc that sits between the ball and socket of the joint can trigger TMJ disorders. Damage to the joint from an impact or blow can also be a contributing factor.
The symptoms associated with TMJ disorders are diverse, but a common thread is discomfort or pain in the jaw region. This pain can radiate to the ear, leading some to mistakenly believe they have an ear infection. Other symptoms to watch out for include:
- Difficulty or discomfort during chewing
- Pain in and around the temporomandibular joint
- A clicking or grating sound when opening or closing the mouth
- A ‘stuck’ or ‘locked’ jaw that limits mouth movements
- Facial fatigue
- Difficulty opening the mouth wide
- Facial swelling
It’s important to note that a clicking or popping sound in the jaw isn’t a definitive sign of a TMJ disorder. If there’s no accompanying pain, treatment may not be necessary. However, if these symptoms persist and intensify, it’s recommended to seek dental consultation for further evaluation and possible treatment.
Addressing TMJ: Dental Treatment Options
The primary goal of TMJ disorder treatment is to alleviate pain and restore normal jaw function. The spectrum of management strategies for TMJ disorders spans from non-invasive therapies and home remedies to dental interventions and surgical procedures, tailored to the severity of the condition.
After a thorough review of the patient’s medical history, physical examination, and diagnostic tests, a customized treatment plan is developed. Treatment typically begins with conservative, less invasive therapies or non-drug measures. If these initial interventions do not provide symptom relief, surgical options may be considered.
It’s important to understand that the success of these treatments varies among individuals, influenced by factors such as the underlying cause of the TMJ disorder, symptom severity, and the patient’s overall health.
Non-Surgical Treatments for TMJ
When it comes to TMJ disorders, non-invasive strategies are typically the first line of defense. These methods can often effectively manage mild cases of TMJ disorders.
- Medications: Simple over-the-counter solutions like nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, can alleviate pain and reduce inflammation. For more severe discomfort, your healthcare provider may recommend stronger analgesics. Low doses of muscle relaxants and antidepressants can also be prescribed to mitigate bruxism and provide pain relief.
- Dental Splints or Mouth Guards: If teeth clenching or grinding is a concern, a dental professional might suggest the use of a soft or hard device fitted over your teeth. These custom-made appliances prevent the upper and lower teeth from contacting each other, thus minimizing the impact of clenching or grinding.
- Physical Therapy: This includes exercises designed to fortify your jaw muscles, along with heat and cold therapy, and ultrasound treatment. These techniques can significantly enhance range of motion and alleviate pain.
- Alternative Therapies: Some individuals find solace in alternative therapies such as acupuncture, relaxation techniques, and biofeedback.
Before embarking on any treatment journey, it’s crucial to discuss the advantages, potential side effects, costs, and expectations with your dentist. Always prioritize conservative, reversible treatments. A cooperative approach to managing your TMJ disorder is key, and involving your doctor in your treatment decisions can be beneficial.
Surgical Treatments for TMJ
In instances where non-surgical treatments fail to provide relief, surgical interventions may be explored. However, it’s advisable to exhaust all non-invasive treatment options first, as surgical solutions are often irreversible. Here are some surgical options:
- Arthrocentesis: This minimally invasive procedure involves the insertion of small needles into the joint to irrigate fluid through the joint, removing debris and inflammatory byproducts.
- TMJ Arthroscopy: In certain cases, arthroscopy can be as effective as open-joint surgery for treating various TMJ disorders. During this procedure, a surgeon inserts a small thin tube (cannula) into the joint space, followed by a small camera (arthroscope) to view the area and assist in diagnosis.
- Modified Condylotomy: This procedure indirectly addresses the TMJ, with the surgery performed on the mandible, not in the joint itself. It can be beneficial for treating pain and if locking is a significant symptom.
- Open-joint Surgery: If your jaw pain persists despite more-conservative treatments and appears to be caused by a structural issue in the joint, your healthcare provider may suggest open-joint surgery (arthrotomy) to repair or replace the joint.
Surgical treatments come with potential risks and complications, including infection, nerve injury, and the possible need for further surgery. Therefore, it’s essential to have a thorough discussion with your healthcare provider about the potential risks and benefits before opting for surgical treatment.
Post-surgical treatment often includes continued physiotherapy to improve flexibility and strength. Your dentist may also recommend continued use of a night guard to maintain your bite and prevent teeth grinding. These measures can contribute to the long-term success of the surgical treatment.
Prevention and Maintenance of TMJ Disorders
The journey to managing TMJ disorders doesn’t end with treatment alone. It’s a two-pronged approach that involves prevention of further occurrences and maintenance of the relief achieved. This involves a blend of lifestyle adjustments, behavioral modifications, and consistent dental visits, all aimed at reducing stress on the jaw joint and muscles. This proactive approach significantly minimizes the risk of developing or aggravating TMJ disorders.
A comprehensive, multi-disciplinary strategy is crucial. This includes self-care at home, dietary modifications, maintaining correct postures, managing stress, and engaging in suitable exercises. These measures not only keep TMJ symptoms at bay but also foster long-term oral health. Dental professionals play a pivotal role in guiding patients through these preventive measures and providing follow-up care to ensure the lasting effectiveness of TMJ treatments.
Regular dental assessments are a cornerstone in this process, facilitating early detection and proactive management of potential issues. In the subsequent sections, we’ll delve into the specifics of lifestyle adaptations, the role of routine dental check-ups, and how dentists weave these elements together for a comprehensive management of TMJ disorders.
Lifestyle Adaptations for Managing TMJ Disorders
Effectively managing TMJ disorders often requires the adoption of certain lifestyle modifications and habits.
- Opt for Soft Foods: Incorporating soft foods like yogurt, mashed potatoes, cottage cheese, soup, scrambled eggs, fruit smoothies, and cooked vegetables into your diet can lessen the strain on your jaw muscles. It’s also advisable to steer clear of hard, crunchy, and chewy foods, and refrain from chewing gum.
- Be Mindful of Clenching and Grinding: Unconscious jaw clenching or teeth grinding, often stress-induced, can exacerbate TMJ disorders. Cultivating awareness and practicing relaxation techniques can make a significant difference.
- Use of Ice or Heat Packs: Applying an ice pack or a warm heat pack to the affected side of your face can offer temporary relief from pain.
- Engage in Exercises: Gentle stretching and relaxation exercises can enhance jaw mobility. Your dentist or physical therapist can guide you to the most suitable exercises for your condition.
- Manage Stress: Since tension and anxiety can trigger TMJ disorders, relaxation techniques such as meditation, deep breathing, and yoga can prove beneficial.
- Maintain Good Posture: Good posture, particularly during activities involving the neck and upper back, ensures optimal alignment of the jaw and neck muscles.
- Limit Extreme Jaw Movements: Try to keep jaw movements moderate to avoid straining your jaw while yawning widely, singing, or yelling.
These lifestyle modifications can alleviate symptoms associated with TMJ disorders and prevent their recurrence. However, it’s crucial that these changes align with the patient’s individual needs and lifestyle for consistency and long-term effectiveness.
Detection and Diagnosis of TMJ Disorders
The journey to managing TMJ disorders begins with accurate detection and diagnosis, a crucial aspect of a dentist’s role. Spotting these disorders early paves the way for prompt intervention, helping to curb or mitigate potential complications.
A comprehensive clinical examination of the jaw is the first step in this process. The dentist will assess the jaw joints for any signs of discomfort or tenderness, listen for unusual sounds like clicks or grating during jaw movement, and evaluate the range of motion in the jaw.
To gain a more detailed view of the temporomandibular joints, imaging procedures such as X-rays, CT scans, or MRI may be recommended. These can provide a cross-sectional image of the jaw and reveal the position of the TMJ disc as the jaw opens and closes.
Bite or occlusion tests are another tool in the dentist’s arsenal. These tests evaluate the alignment and effectiveness of the teeth during jaw movement, with a misaligned bite potentially pointing towards a TMJ disorder.
The diagnostic process also takes into account the patient’s medical history, symptoms, and overall health. This holistic approach ensures a precise diagnosis of TMJ disorders, laying the foundation for a successful treatment plan.
The Role of Dentists in Addressing TMJ Disorders
Dentists play a pivotal role in managing TMJ disorders. Their expertise in oral health equips them with a comprehensive understanding of the entire oral structure, including the temporomandibular joint and surrounding tissues. This knowledge empowers them to diagnose and manage TMJ disorders effectively and holistically.
Their role extends beyond merely treating TMJ symptoms. It encompasses early detection during regular check-ups, proactive care, the implementation of effective treatment plans, and patient education on self-care measures and lifestyle modifications to manage and prevent TMJ symptoms.
In essence, the dentist’s role in managing TMJ disorders is multifaceted. It combines clinical expertise with patient education to provide comprehensive care.