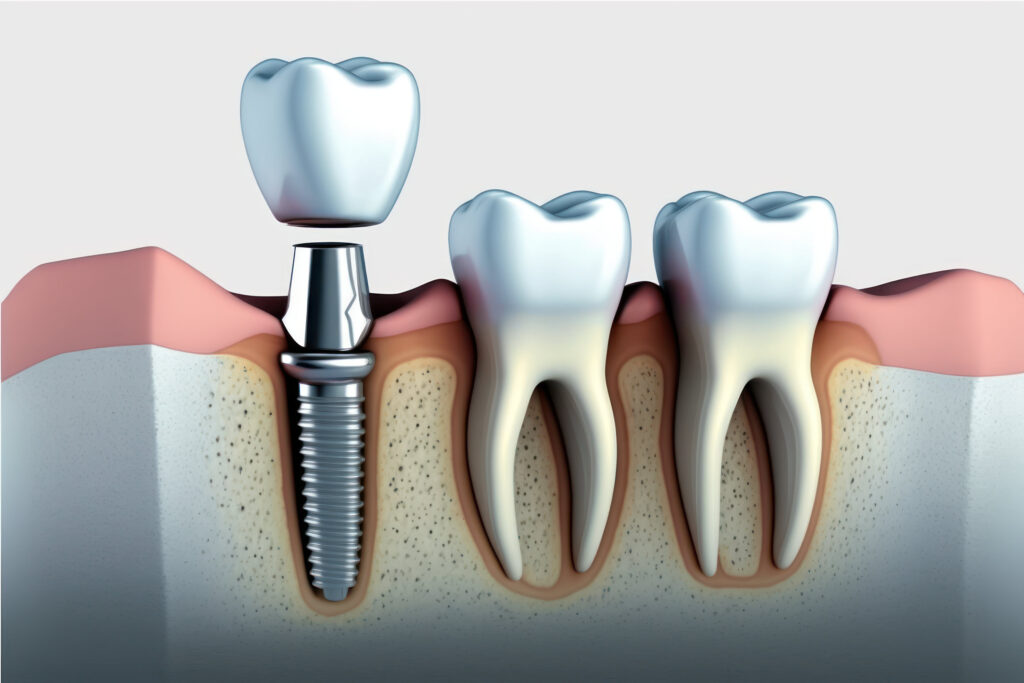
Endosteal implants are a restorative dental solution that addresses tooth loss and facilitates oral rehabilitation. Endosteal implants mimic the structure and function of natural teeth, offering patients grappling with tooth loss a lasting solution.
Tooth loss due to trauma, decay, or other dental conditions can significantly impact an individual’s quality of life. Missing teeth can lead to bone loss in the jaw, difficulties speaking, and poor nutrition. Dental restoration solutions such as endosteal implants can address these challenges by restoring the functionality and aesthetics of a patient’s teeth.
We’ll explore the benefits of endosteal implants, potential risks and complications to consider, and alternative options for individuals who aren’t ideal candidates for endosteal implants.
What Are Endosteal Implants?
An endosteal implant is a dental fixture that’s surgically placed in the jawbone as an artificial root for a replacement tooth. Since endosteal implants are put in the jawbone, they are made from biocompatible materials, such as titanium, to reduce the risk of complications.
Components and materials of endosteal implants include the following:
- Fixture: The fixture is inserted into the jawbone. It’s shaped like a small screw and is usually made of titanium or titanium alloys. Apart from being biocompatible, titanium is durable and easily fuses with the surrounding jawbone
- Abutment: The abutment is connected to the fixture above the gumline. It provides support to the replacement tooth. Abutments can be made of titanium, titanium alloys, or a tooth-colored ceramic such as zirconia
- Prosthesis: This is the replacement tooth or set of teeth that attaches to the abutment. Your dentist can recommend a denture, bridge, or crown depending on the number of missing teeth and your preferences. Replacement teeth can be made of materials that offer aesthetic advantages, such as zirconia and porcelain
Endosteal implants are the most common type of implant for good reason. They offer various advantages over other dental restoration options, including:
- Longevity: Endosteal implants are fused to the jawbone, providing long-lasting support for the replacement tooth. Endosteal implants are also durable. They can last for a lifetime with the proper care.
- Preservation of the jawbone: Jawbone deterioration can occur after tooth loss due to lack of stimulation. Endosteal implants fuse to the jawbone through a process called osseointegration. This process stimulates the jawbone helping maintain its structure and prevent bone loss
- Improved functionality: Endosteal implants provide stable support for the dental prosthetics allowing them to function like natural teeth. Since the implants are fixed to the jaw, they provide a strong biting force and there’s no risk of slipping when chewing
- Natural look and feel: Endosteal implants are designed to function and look like natural teeth. Moreover, the implants can be custom-made to match your natural teeth, ensuring that integrate seamlessly with your smile
Endosteal Implants Requirements vs. Alternatives
Jawbone Requirement
A healthy jawbone is a requirement for endosteal implant placement. Otherwise, the implants won’t provide stable support for the replacement teeth. On the other hand, implant types like subperiosteal and zygomatic implants can be used even with inadequate jawbone structure.
Healing and Integration
Endosteal implants require a healing period to allow the implant to fuse with the surrounding jawbone. This process, known as osseointegration, ensures that the implant is stable and securely embedded in the jaw. Osseointegration for endosteal implants can take several months, while subperiosteal implants have a shorter healing period since they are placed beneath the gum line but on top of the jawbone.
Surgical Procedure
Endosteal implants are surgically placed directly into the jawbone. Other implant types have different designs best suited for specific mouth areas. For example, zygomatic implants are inserted in the zygomatic bone and are recommended when the jawbone cannot support a dental implant.
Suitability
Endosteal implants are a versatile restoration solution that can be recommended for patients with good oral health and a healthy jawbone. Other implant types, such as zygomatic and subperiosteal implants, are best suited for specific cases such as extensive jawbone atrophy and minimal jawbone height.
Comparison of Success Rates and Long-Term Outcomes
Endosteal implants are generally favored because they have a high success rate that ranges from 90% to 95%. Factors such as oral hygiene, bone quality, and implant maintenance play a role in the longevity of the implant. Endosteal implants can last for decades, often exceeding 20 years, with the proper maintenance.
Since subperiosteal implants are placed above the jawbone, they have a lower success rate than endosteal implants, usually ranging from 80% to 90%. As with endosteal implants, subperiosteal implants can last several years with proper maintenance and good oral hygiene.
Transosteal implants have a lower success rate of 70% to 80%. However, they can provide a durable restoration solution for patients who can’t receive endosteal and subperiosteal implants. Due to their complex placement procedure, long-term outcomes of transosteal implants vary. While the implants can last several years, some patients may experience complications requiring additional interventions to correct them.
Factors to Consider When Choosing Between Different Implant Types
When choosing between different implant types, several important factors must be considered. They include the following:
- Surgical procedure: Different implant types have specific surgical placement procedures. For example, the surgical procedure for transosteal implants can only be performed on the lower jawbone. Consult your dentist to understand each implant type’s surgical techniques and potential complications.
- Prosthetic options: Since different implant types have varying prosthetic-support capabilities, it would be best to consider the type of dental prosthetic attached to the implant. For example, fixed dental bridges are commonly used with endosteal implants.
- Cost: Consider your budget when choosing an implant type. Costs can vary depending on the complexity of the procedure, the need for additional treatments, and other factors.
- Longevity: Researching the success rates and longevity of various implant types will help you make an informed decision. For example, endosteal implants have a higher success rate and lower risk of complications compared to transosteal implants.
- Surgeon: Most dentists/ oral surgeons may limit their practice to only offer one type of dental implant option. It is more common that your dentist may only offer endosteal implants and you may need to be referred to a specialist or a dental school if you are interested in alternative implant options.
Endosteal Implant Placement Process
Preoperative Evaluation and Treatment Planning
Your dentist will schedule an initial consultation to evaluate your suitability for implant placement. They may take X-rays and CT scans to evaluate the health of your teeth, gums, and jawbone. Your dentist will also discuss your medical history and expectations for the implant treatment.
Next, they will create a custom treatment plan based on your evaluation results. Your treatment plan will determine preparatory procedures, the number of implants needed, implant positioning, and augmentation procedures like bone grafting if there is insufficient jawbone to support the implant.
Surgical Procedure for Endosteal Implant Placement
Your dentist will discuss anesthesia options before beginning the procedure. Though local anesthesia is commonly used to numb the implant site, they may recommend general anesthesia for an extensive and complex procedure or if you have severe dental anxiety.
After ensuring the anesthesia has taken effect, your dentist will expose the underlying jawbone by making a small incision in the gum tissue. They will then prepare a pilot hole at the implant site using dental drills with increasing sizes. The special drills gradually widen the pilot hole to match the size and dimensions of the implant.
Once the pilot hole is ready, your dentist will carefully insert the implant into the jawbone. They may use a restorative torque to ensure the implant is stable and fixed.
Healing Period
A healing period is necessary after the implant placement to ensure osseointegration occurs. Osseointegration is the process by which the implant fuses with the surrounding jawbone. Depending on the jawbone quality, implants placed, and your overall health, the process may take a few weeks to several months. The standard healing period is anywhere between 3 and 6 months.
Abutment Placement
Your dentist may perform a minor surgical procedure to attach an abutment after successful osseointegration. The procedure involves exposing the top of the implant and attaching an abutment where the dental prosthesis will be placed. A digital scan or impression that will be used to fabricate the final prosthesis may be taken at this appointment or a couple of weeks after this appointment. A temporary prosthesis may also be placed during this appointment.
Prosthesis Placement
Once the gum tissue around the abutment has healed and your permanent prosthesis has returned from the lab, your dentist will schedule a prosthesis placement appointment. Depending on your treatment plan and the number of missing teeth, the final prosthesis may be a denture, crown, or bridge. After placing the prosthesis, your dentist will provide you with aftercare instructions and schedule follow-up appointments to monitor the healing process of the implant.
Cost Considerations for Endosteal Implants
Here are some key factors that can impact the cost of endosteal implants:
- Dentist’s expertise/region: Endosteal implant placement is a complex procedure which means that highly skilled and experienced dentists may charge more for their service.
- Implant material: While endosteal implants are primarily made of titanium, quality and design variations may affect the price of different implants.
- Number of implants: Since endosteal implant cost is determined per implant, the number of implants required for your dental restoration will affect the total cost of the procedure.
- Preparatory procedures: Sinus lifts, CT scans, bone grafting, surgical guides, and tooth extractions are some of the preparatory procedures that may be necessary before implant placement. These procedures can increase the overall cost.
- Region: Depending on where you are in the country or your state, dental implant services may cost more in some metropolitan areas.
Comparison of Endosteal Implant Costs with Other Dental Restoration Options
When comparing endosteal implant costs with other restoration options, it’s crucial to consider oral health benefits, aesthetics, and longevity. For example, dentures are more affordable than endosteal implants. However, they have a shorter lifespan than implants and may require frequent adjustments.
On the other hand, dental bridges are fixed restorations that are typically less expensive than implants. However, dental bridges can’t prevent bone loss since they cannot stimulate the jawbone. Also, placing dental bridges may require the alteration of healthy teeth.
Though endosteal implants have a higher upfront cost, their long-term benefits are worth the expense. Implants stimulate the jawbone, prevent adjacent teeth from shifting and restore natural chewing function.
Consult your dentist about financing options and whether your insurance plan covers the procedure. These options can significantly lower the cost of implant placement.
Success Rates and Safety of Endosteal Implants
Research and Statistics on the Success Rates of Endosteal Implants
Exhaustive studies have shown that endosteal implants have high success rates and longevity. For instance, a systematic review published in the International Journal of Oral and Maxillofacial Implants in 2019 revealed that the cumulative survival rate of endosteal implants over five years ranged from 90% to 96%.
Another study published in the Journal of Dental Research in 2014 analyzed the longevity of dental implants over ten years. It found that endosteal implants had a cumulative success rate of 94.6%
Factors Influencing the Long-Term Success of Endosteal Implants
The factors mentioned below can influence the long-term success of endosteal implants.
- Osseointegration: It’s crucial that the implant completely fuses with the jawbone to ensure its longevity. Your jawbone health and the implant’s surface can affect the osseointegration process
- Implant design: Implant quality and design significantly affect the long-term success of endosteal implants. For example, implants made of titanium and titanium alloys are durable, lightweight, and more likely to fuse with the surrounding jaw bone
- Patient’s health: Health conditions such as uncontrolled diabetes and autoimmune diseases can negatively affect implant integration. Also, lifestyle choices like smoking can hinder healing and limit the implant’s longevity
- Oral hygiene practices: Poor oral hygiene can lead to peri-implantitis, which causes implant failure. As such, good oral hygiene practices and regular dental cleanings play a crucial role in implant success
Safety Considerations and Potential Complications
While endosteal implants are generally considered safe and successful, you should be aware of some safety considerations and potential complications. They include the following:
- Osseointegration complications: Osseointegration can be negatively affected by excessive smoking, systematic conditions like diabetes, and certain medications. Osseointegration issues can lead to implant failure
- Infection: An infection at the implant site can lead to complications. However, your dentist will take precautions, such as sterilization, to minimize the risk of infection during the procedure. Also, good oral hygiene habits play a crucial role in preventing infection after the procedure
- Nerve damage: Poor implant placement technique can damage nearby nerves, such as the inferior alveolar nerve in the lower jaw and the infraorbital nerve in the upper jaw. Nerve damage can lead to numbness and tingling in the affected area.
- Sinus complications: Implants placed in the upper jaw can disrupt the sinus membrane leading to sinus infections and other sinus-related complications such as sinusitis
Considerations and Limitations of Endosteal Implants
Bone Quality and Quantity Requirements for Endosteal Implants
Bone quality refers to the density and strength of the jawbone. Sufficient jawbone density is crucial to provide stability and support for the implant. Low bone density caused by long-term tooth loss or osteoporosis increases the risk of implant failure.
Bone quantity refers to the available volume and height of the jawbone that can accommodate the implant. The jawbone should have adequate bone volume to accommodate the implant and ensure osseointegration.
Contraindications and Limitations of Endosteal Implant Placement
Like any dental restoration solution, endosteal implants have certain contraindications and limitations that you should consider. They include the following:
- Insufficient bone quantity or quality: Severe bone loss in the jaw or poor bone quality can increase the chance of implant failure. In such cases, your dentist may recommend bone grafting or alternative restoration solutions
- Periodontal disease: Active periodontal disease can cause bone loss around the teeth and compromise the success rate of dental implants. As such, treating periodontal disease is necessary before placing endosteal implants
- Systemic diseases: Certain systemic diseases can limit a patient’s viability for endosteal implant placement. For example, uncontrolled diabetes affects the body’s ability to heal and increases the risk of implant failure
- Smoking and tobacco use: Cigarettes and tobacco products contain various chemicals that hinder healing and increase the risk of implant failure. As such, dentists recommend quitting smoking before the patient can consider implant placement
Alternative Options for Individuals with Inadequate Bone Structure
- Pterygoid implants: Pterygoid implants provide an alternative for patients with severe bone loss in the posterior maxillary region. The implants are placed in the pterygoid bone located in the back of the maxilla
- Zygomatic implants: Zygomatic implants are attached to the zygomatic bone to provide a stable foundation for dental restorations. They provide an alternative for patients with an inadequate upper jaw
- Subperiosteal implants: Subperiosteal implants provide an alternative for patients with inadequate bone height. They are placed beneath the gum line but above the jawbone. Subperiosteal implants are designed to be held in place by the jawbone and surrounding tissues
- Mini Dental Implants (MDIs): MDIs are designed for patients with limited bone availability. They are smaller in diameter than traditional implants and can be used to support dentures and crowns
Recovery and Aftercare
Postoperative Instructions and Care For Endosteal Implants
Following postoperative instructions as your dentist recommends ensures proper healing and longevity of the implant. Here are some general aftercare guidelines:
- Oral Hygiene: Use a soft-bristled toothbrush to clean your teeth at least twice daily. Avoid brushing the implant site for the first few days. Instead, rinse your mouth with antimicrobial mouthwash or warm salty water
- Medication: Take prescribed medication, such as antibiotics, as your dentist recommends. Complete the dose to prevent infection and other complications
- Diet: Avoid hot, hard, or spicy foods for the first few days after the surgery since they irritate the implant site. Instead, stick to soft and cool foods and gradually introduce solid foods as you heal.
- Pain management: It’s normal to experience pain and discomfort after the surgery. Your dentist will prescribe over-the-counter medication to manage pain and reduce discomfort. You can also apply ice packs to the cheek for the first 24 hours to reduce swelling
- Bleeding: Like with most dental surgical procedures, you’ll experience minor bleeding from the implant site for the first few days. You can control the bleeding by placing a clean gauze pad over the surgical site and gently biting down on it. However, you should contact your dentist if the bleeding persists.
- Tobacco and Alcohol: Consuming alcohol and using tobacco products during the healing period can increase the risk of complications and contribute to implant failure. For example, cigarette smoke can irritate the surgical site and hinder healing.
- Long-term maintenance and follow-up care: Regular dental check-ups, professional cleaning, and implant stability assessment are vital aspects of long-term maintenance for endosteal implants. Attending follow-up appointments as scheduled by your dentist is crucial to ensuring the implant’s longevity and preventing complications such as peri-implantitis.
Types of Endosteal Implants
Endosteal implant types can be categorized based on design, materials, and surgical technique. Here’s an overview of the most common types:
- Root-form implants: These are screw-shaped implants designed to mimic the functionality of natural teeth roots. Their design allows them to provide stability and support for dental prosthetics
- Plate-form implants: Plate-form implants are blade-shaped and are used when the jawbone is too narrow to support a root-form implant. They are placed horizontally into the jawbone and are made of biocompatible materials such as titanium
- Mini implants: These implants have a smaller diameter than traditional implants, making them an ideal choice in cases with limited bone density or space
- All-on-4 implants: All-on-4 implants are four implants strategically placed in the jawbone to support a full arch of teeth. These implants are typically recommended for patients with significant tooth loss
It’s important to note that your dentist will recommend the most suitable implant type after evaluating your oral health, bone structure, and medical history.
Endosteal implants have proven to be a highly effective dental restoration solution with various advantages, including their durability, stability, and natural appearance. Endosteal implants allow patients grappling with tooth loss to regain their ability to chew and speak comfortably.
It would be best to consult a dental professional when considering endosteal implants. A qualified dentist will create a customized treatment plan tailored to your oral health needs.
However, it is essential to stress the importance of regular check-ups, good oral hygiene habits, and following post-implant aftercare instructions. These practices will improve the long-term success and longevity of endosteal implants.