Disclaimer: This article is for informational purposes only. O2 Dental Group does not offer subperiosteal implants. We only offer the endosteal implant procedure.
Subperiosteal implants are a dental restoration treatment used to replace missing teeth for patients who may not be suitable for traditional dental implants. Unlike traditional implants, subperiosteal implants are placed beneath the gum line and on the jawbone. As such, they provide a viable alternative for patients with insufficient jaw bone density.
Subperiosteal implants can address the challenges caused by tooth loss, such as poor nutrition, bone resorption, and speech impairment. This article covers all the crucial aspects of subperiosteal implants, including the placement process, advantages over other dental restoration options, limitations, and alternative options for individuals with specific dental conditions.
What Are Subperiosteal Implants
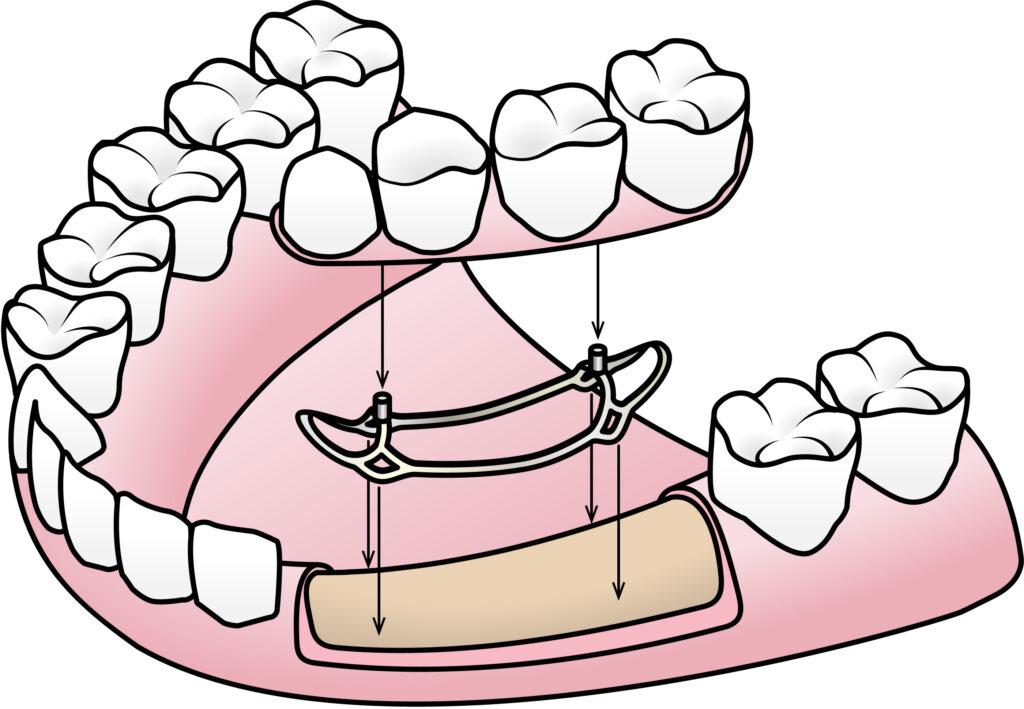
Subperiosteal implants are a dental restoration option used to replace missing teeth when a patient has insufficient jaw bone density. The implants utilize a titanium custom framework designed to fit the patient’s jaw. Posts or abutments protruding from the gum line provide support for the artificial teeth.
Advantages of Subperiosteal Implants over Other Dental Restoration Options
- Minimally invasive procedure: Subperiosteal implants are placed on top of the jawbone, removing the need for invasive procedures such as bone grafting or drilling the jawbone
- Suitable for patients with insufficient bone density: Subperiosteal implants are an ideal dental restoration option for patients with inadequate bone height or width. They are custom-made to fit the patient’s jaw bone, eliminating the need for a dense bone structure
- Versatility: Subperiosteal implants can be used to replace multiple missing teeth. The implants also support dental prostheses, including partial or full arch dentures and single crowns, and a dental bridge.
- Stable and durable: Subperiosteal implants rest over the jawbone providing stable support for the replacement teeth and reducing the risk of slippage. They can also last for several years with proper care and maintenance
- Faster healing time: Subperiosteal implants involve a minimally invasive procedure compared to endosteal and transosteal implants, resulting in less discomfort and a quicker recovery period for the patient
Subperiosteal Implants vs. Regular Implants
Key Differences between Subperiosteal Implants and Other Implant Types
Surgical Procedure
The surgical placement procedure of subperiosteal implants involves making an incision on the gumline and placing a custom-made metal framework over the jawbone. The gum tissue covers the metal framework and provides additional support once it heals. The metal posts protruding through the gum tissue provide support for the replacement teeth.
Endosteal and transosteal implants also require a surgical procedure. However, the implant post is inserted into a hole drilled in the jawbone and allowed to integrate with the surrounding bone for several months. Dental prostheses are placed on the implant once the integration period (osseointegration) is complete.
Bone Requirement
Since subperiosteal implants are placed over the jawbone, they benefit patients with inadequate bone density. Conversely, a healthy jawbone is a requirement for receiving traditional implants. Sufficient bone height and width are necessary to support endosteal and transosteal implants.
Healing and Recovery Time
Patients receiving a subperiosteal implant may experience a shorter recovery period due to its minimally invasive surgical procedure. Osseointegration takes less time since the implant is placed on the jawbone.
On the other hand, surgical procedures for implant types such as endosteal and zygomatic implants are more extensive and invasive compared to subperiosteal implants. For example, zygomatic implants involve inserting posts into the zygomatic bone to support the replacement teeth. As a result, the implants require an extended healing period to fuse with the surrounding bone properly.
Cost
Though subperiosteal implants have high success rates in patients with inadequate jawbone density, they may cost more than regular implants. The expertise required to place the implants and the custom fabrication of the metal framework adds to the overall cost.
However, regular implants may cost more than subperiosteal implants in some cases. For example, since endosteal implants are charged per implant, they may cost more if you have multiple teeth replaced. Moreover, additional procedures like bone grafting can significantly increase the overall cost of endosteal implants.
Comparison of Success Rates and Long-Term Outcomes
While subperiosteal implants are an effective dental restoration solution, they have lower success rates than regular implants. It’s important to note that factors like the patient’s bone quality, the dentist’s expertise, and the implant’s shape and size can affect the success rate of subperiosteal implants.
Furthermore, subperiosteal implants generally have positive long-term outcomes but may not be as durable as regular implants. While improvements in implant design have improved their durability, subperiosteal implants may be less stable and prone to complications over time due to their placement over the jawbone.
Factors to Consider When Choosing Between Different Implant Types
- Surgical technique: It’s important to consider the surgical technique when choosing an implant as it affects the treatment timeline and healing process. For example, endosteal implants require a two-step procedure with a long osseointegration period before the dental prosthesis can be attached. On the other hand, the healing period for subperiosteal implants is typically shorter since the surgical procedure doesn’t involve drilling into the bone
- Material: While dental implants are typically made from titanium, a biocompatible material, It would be best to consult your dentist on its pros and cons and whether you may develop allergic reactions
- Cost: Consider your budget and insurance coverage when choosing an implant type. For example, while zirconia implants are known for their aesthetic advantages, they may cost more than titanium implants. Moreover, the complexity of the implant procedure can add to the overall cost.
- Overall health and medical history: Certain systemic diseases and health conditions can affect the success of dental implants. For example, diabetic patients are less likely to receive endosteal implants as the condition can significantly delay the healing process and increase the chance of implant failure
Subperiosteal Implant Placement Process
Preoperative Evaluation and Treatment Planning
The subperiosteal implant placement process starts with a consultation with your dentist. They will thoroughly evaluate your oral health to assess the condition of your teeth, gums, and jawbone. X-rays and CT scans are particularly beneficial for determining the bone quality in the treatment area.
Your dentist will also discuss your dental history, desired outcome for the procedure, and any existing medical conditions before developing a custom treatment plan.
Preoperative Procedures
Your dentist may perform preoperative procedures to reduce the risk of implant failure and increase the chances of successful integration. These procedures depend on your evaluation results. For example, your dentist may have to address gum disease or oral infections before implant placement.
Impressions and Imaging
Next, your dentist will take impressions of your jawbone to capture its shape and contours using dental putty or digital scanning technology. The impressions provide an accurate model for fabricating the custom implant framework. Some dental practices use advanced imaging techniques like CT scans to create detailed 3D images of your jawbone that aid in planning the ideal placement of the subperiosteal implant.
Framework Fabrication
The impressions are sent to a dental laboratory where skilled technicians will fabricate a custom implant framework that matches the shape and size of your jawbone. The framework is made of titanium since it’s biocompatible, light, and durable.
Implant Placement Surgery
Your dentist will administer local anesthesia to ensure your comfort during the surgery. They will then make a small incision in the gum tissue to expose the underlying jawbone and carefully position the custom-made framework. Small screws and other attachment mechanisms may be used to secure the framework. Your dentist will suture the gums back in place and provide you with aftercare instructions to promote healing.
Healing and Integration
Depending on your jawbone quality, oral health, and care routine, the treatment site might take three to six months to heal and integrate with the underlying jawbone. Your dentist will schedule regular appointments to monitor the healing process, address complications, should any arise, and ensure proper integration.
Once your gums have healed, your dentist will install implant posts onto the frame where the dental prosthetic will be attached.
Cost Considerations for Subperiosteal Implants
Factors Influencing the Cost of Subperiosteal Implants
The cost of subperiosteal implants can vary depending on several factors. They include the following:
- Dentist’s experience and skill: Since placing subperiosteal implants requires extensive dental expertise and specialized training, skilled dentists may charge more for their services
- Diagnostic tests and imaging: Diagnostic tests such as X-rays and CT scans aid in assessing your jawbone health before implant placement. Additionally, 3D imaging may be necessary to ensure proper placement and accurate framework fabrication. These tests can affect the overall cost of the procedure
- Additional treatments: Depending on your oral health, your dentist may perform additional treatments. For example, oral infection or gum disease cases must be addressed before implant placement. These procedures can add to the overall cost.
- Dental insurance coverage: Your insurance coverage can offset the cost of subperiosteal implants. Some plans may cover a portion of the cost, helping reduce out-of-pocket expenses.
Comparison of Subperiosteal Implant Costs with Other Dental Restoration Options
At a glance, it’s clear that subperiosteal implants may cost more than some dental restoration options. However, it’s important to consider the various benefits that subperiosteal implants have over other restoration options.
For instance, dental bridges may be a slightly cheaper option for replacing one or more missing teeth, but placing dental bridges may require the alteration of healthy teeth. Furthermore, subperiosteal implants are more stable and provide a stronger foundation for dental prosthetics than dental bridges.
Partials may offer a cheaper restoration alternative. While they effectively restore tooth functionality, partials tend to be more uncomfortable and don’t fit into most patient’s lifestyles. Moreover, the patient may require root canal therapy if the dental crown inflames the tooth’s pulp, adding to the overall cost of the procedure.
The bottom line is that subperiosteal implants are worth the cost, considering their longevity, success rate, and oral health benefits. Additionally, insurance coverage and financing options can help make the cost of subperiosteal implants more affordable.
Success Rates and Safety of Subperiosteal Implants
Research and Statistics on the Success Rates of Subperiosteal Implants
The success rate of subperiosteal implants can vary depending on the patient’s oral health, implant design, materials, and surface coatings. However, various studies have shown that subperiosteal implants have a high success rate.
For example, a study published in the Journal of Oral and Dental Health Research showed that the survival rate of subperiosteal implants was 98% over seven years. Another study researching custom-made laser sintering subperiosteal implants reported a success rate of 95.8% over two years.
Factors Influencing the Long-Term Success of Subperiosteal Implants
The following factors can influence the long-term success of subperiosteal implants:
- Jawbone health: Though subperiosteal implants are recommended for patients who can’t receive traditional implants due to inadequate jaw bone density, a healthy jawbone is necessary to support and stabilize the custom metal framework.
- Patient’s overall health: The patient’s overall health can determine the longevity of subperiosteal implants. For example, systemic conditions such as diabetes can hinder the healing process and increase the risk of implant failure
- Surgical technique: Proper placement of subperiosteal implants requires extensive experience and specialized training. Precise positioning of the implant, along with skillful surgical technique, can impact the longevity of the implant
- Oral hygiene routine: Good oral hygiene habits such as regular brushing and flossing can reduce the risk of implant failure by preventing peri-implantitis and other oral infections
- Follow-up care: Attending follow-up appointments set by your dentist can significantly impact the long-term success of your subperiosteal implant. Routine examinations will help your dentist monitor your implant and perform early treatment for potential issues
Safety Considerations and Potential Complications
Though subperiosteal implants are a viable dental restoration treatment for patients with inadequate bone density, you should consider its potential complications. Here are some key points to keep in mind:
- Infection: As with any surgical procedure, there’s a risk of infection after subperiosteal implant placement. Poor oral hygiene and lifestyle habits such as smoking can significantly increase the risk of infection and implant failure
- Bone resorption: Since subperiosteal implants can’t stimulate the jawbone, bone resorption can occur over time. The bone loss can affect the stability of the implant and may require additional treatments to restore its functionality
- Surgical risks: While subperiosteal implant placement requires minimal surgery, general surgical risks are involved. These include nerve damage, sinus compilations, bleeding, and damage to the adjacent teeth.
- Healing complications: Subperiosteal implants require proper healing to support the dental prosthetic. However, inadequate postoperative care, health complications, and destructive habits such as smoking, can hinder the healing process and contribute to implant failure
Considerations and Limitations of Subperiosteal Implants
Suitable Candidates for Subperiosteal Implants
Suitable candidates for subperiosteal implants include patients who:
- Suffer from bone resorption: Bone loss in the jaw can occur due to factors such as aging, tooth loss, and severe periodontal disease. Subperiosteal implants are particularly beneficial for patients with significant bone resorption since they may not be suitable for traditional implants
- Have inadequate jawbone density: Endosteal implants require sufficient bone density for support. Since subperiosteal implants are placed over the jawbone, they are an ideal dental restoration alternative for patients with insufficient jawbone structure
- Cannot undergo bone grafting: Some patients may not be ideal candidates for a dental bone graft. In such cases, subperiosteal implants can be a viable solution for replacing missing teeth
- Prefer a non-invasive procedure: Subperiosteal implant placement is less invasive than other implant placement procedures. They don’t require extensive bone preparation, making them an ideal option for patients who desire a relatively non-invasive procedure
Contraindications and Limitations of Subperiosteal Implant Placement
Inadequate Alveolar Ridge Width
The alveolar ridge is a bony ridge that holds the sockets of the teeth. The ridge is crucial to subperiosteal implants since it supports the implant framework. An alveolar ridge with an inadequate width won’t provide enough support for the framework, increasing the chance of implant failure.
Uncontrolled Systemic Conditions
Patients with autoimmune disorders and systemic conditions, such as diabetes, may not be ideal candidates for subperiosteal implants. These conditions hinder healing, impair osseointegration, and increase the risk of implant failure.
Active Periodontal Disease
Periodontitis affects the gums and damages supporting structures around the teeth. Periodontal disease increases the risk of implant failure and infections such as peri-implantitis. Successful treatment of active periodontal disease is necessary before placing subperiosteal implants.
Insufficient Bone Height
Though subperiosteal implants are recommended for patients with inadequate jaw bone density, they require a certain bone height for successful placement. Insufficient bone height and poor bone quality can lead to complications and compromise the success of the implants.
Alternative Options for Individuals with Specific Dental Conditions
- Zygomatic implants: Patients with severe bone loss in the upper jaw may not be suitable candidates for subperiosteal implants. In such cases, zygomatic implants can be a viable restoration alternative. These implants are anchored in the cheekbone to provide a stable foundation for dental prosthetics
- Mini dental implants: Minimal dental implants are often recommended for patients who lack the sufficient bone density or height necessary for subperiosteal implants. They are less invasive and have a smaller diameter than endosteal implants.
- All-on-4 implants: Though subperiosteal implants can replace multiple missing teeth, all-on-4 implants can provide a more cost-effective alternative. These implants can be placed in a single procedure and support a full arch of teeth (usually four or six).
Subperiosteal Implant Recovery and Aftercare
Postoperative Instructions and Care For Subperiosteal Implants
While your dentist will provide specific aftercare instructions based on your circumstances, the following general postoperative instructions can help ensure proper healing and reduce the risk of implant failure:
- Maintain oral hygiene: Good oral hygiene reduces the risk of infection and complications during the healing period. However, you should avoid brushing the treatment site for the first few days. Gently rinsing your mouth with salty water will soothe the surgical site and keep it clean.
- Avoid smoking and alcohol: Cigarette smoke and alcohol can hinder healing and irritate the surgical site. As such, you should avoid smoking and limit alcohol consumption during the healing period
- Follow your dentist’s instructions: Your dentist will provide personalized aftercare instructions after the procedure. Carefully follow these instructions to ensure proper healing and reduce the risk of complications
- Follow a soft diet: Avoid hard and crunchy foods as you heal. Instead, stick to a soft diet consisting of foods like applesauce, yogurt, mashed potatoes, smoothies, and soups
- Manage swelling and discomfort: As with any dental surgical procedure, it’s normal to experience swelling, discomfort, and bleeding after implant placement. Your dentist will recommend over-the-counter painkillers to manage pain and discomfort. Also, regularly applying an ice pack to the affected area can help reduce swelling and alleviate discomfort.
Subperiosteal implants are an effective dental restoration solution that particularly benefits patients with insufficient bone structure to support traditional implants. Subperiosteal implants have various benefits, including eliminating the need for costly bone grafting procedures, improving aesthetics, and restoring chewing and speech function.
Consult your dentist if you’re considering subperiosteal implants. They will offer more information on the procedure, including its risks and benefits. Your dentist will also assess your viability for the procedure and create a treatment plan based on your unique oral health needs.